'It has been a trauma': nurses on 'shambolic' 111 Covid-19 clinical service
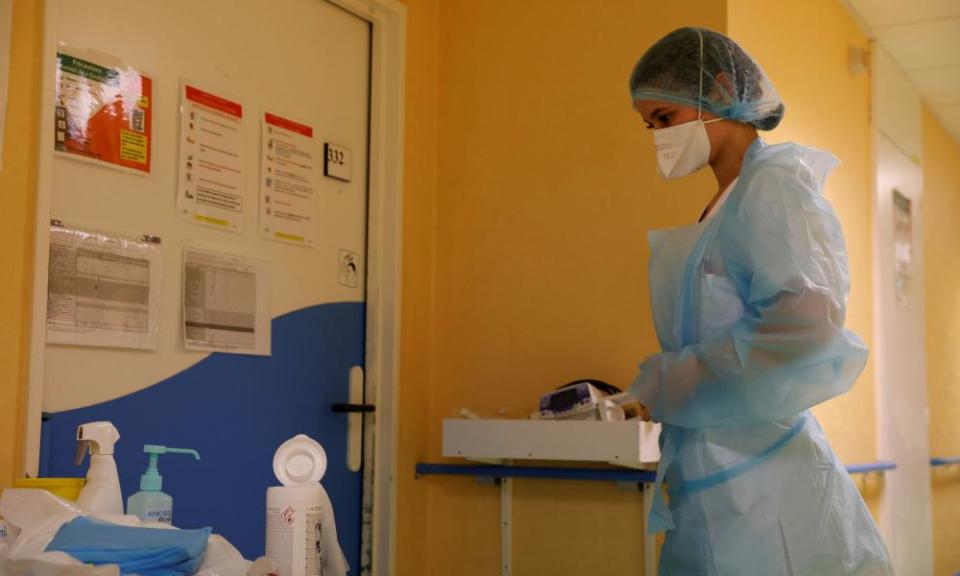
Ten nurses who worked for the NHS 111 Covid-19 Clinical Assessment Service have come forward to blow the whistle on their unit’s organisation, describing it as shambolic, and lacking in adequate training and safeguards.
The nurses, who had retired or left the NHS after many years’ experience, were recruited to the CCAS, a new national division of NHS 111, after the health secretary, Matt Hancock, urged doctors and nurses to return and work on the response to the pandemic.
The former CCAS nurses came forward to talk about their experiences after it was revealed that an audit had found that 60% of calls to patients, by nurses and allied healthcare professionals (AHPs), had not been safe.
The nurses, who asked not to be identified, told the Guardian that they were offered their positions on the CCAS without having an interview, then were given negligible training, no mentoring and inadequate supervision or support.
The role required them to call patients who had been identified by the 111 service to have coronavirus symptoms, and to make clinical assessments about how ill they were and whether they needed medical attention.
“Nurses don’t have training in diagnosis and clinical decision-making, so I thought there would be a lot of training for the CCAS, but there wasn’t,” one of the nurses said. “I’m NHS through and through, but some basics of NHS organisation went by the wayside; they put people into critical roles without proper training. Once I understood the structure, I didn’t think it was safe.”
The nurses explained that throughout long NHS careers in different disciplines, their work did not involve medical diagnosis, making critical decisions about a patient’s condition, or triage. Yet only four hours of training were given for the CCAS.
“I had no interview,” another of the nurses said. “I did the four hours training – you couldn’t actually do it in four hours, but we were only paid for four – then went on to make calls to people. They had been triaged as having Covid, but it could be anything.
“The nurses did so much extra reading and accessed resources, to be as prepared as possible. But there was no script for talking to people, we weren’t given red flags to be aware of, no instruction. There was no structure of clinical support or a supervisory doctor on a shift to whom we could turn or transfer a call if we were out of our depth.”
Since the start of the pandemic, the government and NHS have directed people to use the 111 service if they fear they have coronavirus symptoms, to help keep GPs and hospitals clear to cope with more serious cases. NHS England says 111 has helped millions of people receive the right care and advice, and that recruits were “carefully selected, screened and trained.”
But in recent weeks the Guardian has uncovered alarming questions about the 111 service, including over the level of training provided to initial call handlers in the new Coronavirus Response Service – set up by by South Central Ambulance Service (SCAS) – and the initial advice given.
The Covid-19 Bereaved Families for Justice Group estimates that a fifth of its 2,000 members’ relatives died after calling 111 and being told by an initial call handler that they were safe to stay at home.
In the CCAS, the clinical part of the operation run by SCAS, after some calls were audited, many nurses and AHPs raised concerns themselves, saying they did not have the required skills or training . They were then “paused” while further audits of calls were carried out.
In an email sent on 3 July, the clinical assurance director of SCAS’s National Covid-19 Pandemic Response Service said the audits had raised concerns about their safety.
An intensive audit was then conducted, with the result, communicated in a 14 August email, that “over 60% of calls have not passed the criteria demonstrating a safe call”.
The nurses were told that their work for the CCAS would be terminated on 30 September, and were invited to complete the full SCAS four to six week training and qualification process for working within NHS 111.
One of the nurses reflected: “What was the point of offering the training at the end, and almost nothing at the beginning? People’s lives are at stake, you can’t do it in retrospect.”
SCAS told the Guardian there had been 28 nurses actively working on CCAS, 1.4% of the total employees. It is now entirely staffed by GPs and medical staff.
“Those nurses were accountable under their professional code of conduct, which clearly states that they should work within their clinical competency,” SCAS said in a statement. “Specifically each nurse was required to sign a declaration against a set of competencies stating that they considered themselves safe to practice within the CCAS.”
SCAS said governance had been established for the service “in line with CQC and NHS England requirements,” including call audits, and that: “Every individual who had calls audited received feedback.” The “clinical incidents and concerns” identified by the audits had been fully investigated, SCAS said, and one classed as a “serious untoward incident” had “caused no harm to the patient. The CCAS remains an important, safe and critical service for patients during the pandemic.”
One of the nurses said: “We came out of retirement to help, and took on the role in good faith, not realising the lack of support, clear leadership and mentoring.”
Another said: “I had a long and successful career in the NHS, but this was shambolic. We are all educated, caring, experienced people, but after coming back to help in the pandemic, now I feel very disheartened; it nags away at me. It has been a trauma.”

 Yahoo Finance
Yahoo Finance 