Hospitals itch to ramp up elective surgery amid coronavirus profit crunch
The health care industry is struggling from the economic effects of the coronavirus pandemic: Hospitals and insurance companies are facing revenue shortfalls as a result of the number of patients being treated for the coronavirus.
Insurance companies are covering costs of treatment and testing for COVID-19, the disease caused by coronavirus, while hospitals have had to cancel elective procedures in order to maintain supply of personal protective equipment (PPE). And since these elective procedures are one of the main sources of revenue for hospitals, these hospitals are facing a cash crunch like never before.

“You’ve never seen this kind of decline in utilization,” John Ransom, managing director of equity research at Raymond James, told Yahoo Finance.
A report from the American Hospital Association (AHA) estimated a loss of $202.6 billion for America’s hospitals and health systems between March 1, 2020 to June 30, 2020. That translates to an average financial impact of $50.7 billion per month.
And an analysis by TransUnion found that over 500 hospitals experienced visitor declines between 32%-60%, just in the month of March alone, largely because hospitals reportedly earn approximately $700 more on each elective admission than on each emergency department admission.
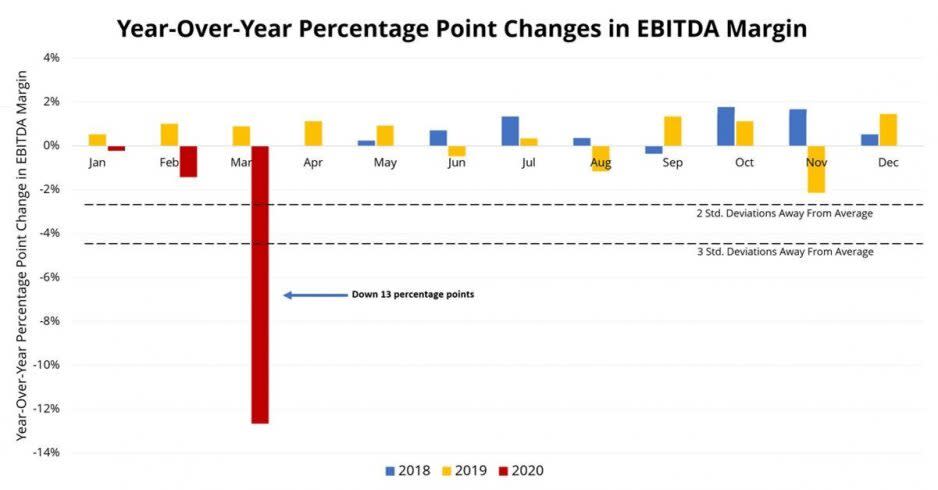
“From a hospital standpoint, these procedures represent anywhere from 40 to 60% of their overall revenue,” Jonathan Wiik, principal of healthcare strategy at TransUnion Healthcare, told Yahoo Finance.
Typically, he said, “this patient population has insurance. They’re electively scheduled procedures, so they’ve been financially cleared upstream a long time ago by their orthopedist or their cardiologist, so they’ve had an X-ray and labs, and they’ve been in to see the doc, and they scheduled this procedure. They’re typically ‘funded’ and they help subsidize lots of other things that aren’t funded like emergencies and shortfalls in payment from Medicaid, so it’s kind of a double whammy for hospitals.”
Cost-cutting measures
Some hospitals are already seeing the effects of the profit crunch and are having to resort to cost-cutting measures.
“It puts a severe cash flow strain on the hospital because 40% of your top-line revenue is no longer there,” Daniel Steingart, vice president at Moody’s, told Yahoo Finance. “The interruption in cash flow puts a significant stress on the entire system.”
Johns Hopkins University, one of the largest health systems in the country, announced last month that it would be implementing salary freezes, hiring freezes, and retirement contribution suspensions. The hospital was originally projected to bring in $72 million, but it’s now expecting to lose $100 million this year.
Boston Medical Center is furloughing approximately 700 people (10% of its staff), while the Medical University of South Carolina in Charleston is laying off 900 people (not including front-line workers) and asking full-time employees to take a 15% salary cut.
Aside from furloughs, salary cuts, and layoffs, another measure hospitals could take is upping the price of certain procedures and treatments, which insurance companies pay for their enrollees. With these companies already facing the coronavirus health shock, they could then increase the price of premiums and deductibles in order to recoup some of the losses.
“There’s this deficit, so insurance companies had a very profitable first quarter,” Wiik said. “They will probably have a similar repeat in Q2. I’m not a financial analyst, but just knowing the numbers, I think they haven’t had exposure from a claims risk standpoint because of the elective procedures. They most certainly have had exposures from the COVID standpoint in cases and have said that may or may not impact premium increases going forward.”
According to an actuarial brief from Covered California, premiums for 2021 could increase from anywhere between 4% to more than 40% as a result of COVID-19.
The CARES Act passed by Congress back in March allocates some funds to go towards health care providers facing financial pressures. But only a portion of it goes towards hospitals, and its intent is to keep the hospitals functioning, rather than fully restoring things back to normal.
‘Older generations are the least likely to come back’
Even if hospitals are able to resume all of their elective procedures, will people actually be willing to come in to have them done? And will that be enough to recoup all of the losses?
According to Steingart, the answer is: “not entirely and not right away.”
“On one hand, anybody who had something that was delayed or postponed for surgery or procedure or visit, whatever, yes, they can come back into the system, assuming they still have insurance,” he said. “Take Medicare, which is round numbers, about half of hospital patients and revenue.”

Steingart continued: “Those folks have obviously not lost insurance if they’re covered by Medicare, but getting them back into the system, it doesn’t happen overnight. Let’s say you have two and a half months of backlogged, deferred care. There’s a limit to how much extra the hospital system can bring through in a given period of time.”
The TransUnion survey found that 27% of consumer’s elective procedures were cancelled or delayed as a result of the pandemic. Furthermore, 49% of these consumers may be hesitant to reschedule their procedures, at least until the risk of infection decreases more.
“Younger generations are probably more apt to come back, but are the least risk, and the older generations are the least likely to come back or are coming back at the slowest and have the highest risk,” Wiik said. “That’s going to be something that the hospitals and providers are going to have to navigate from their engagement strategies, because the populations they need to get back there are probably the highest risk. They’re the least likely to come back based off of this survey and their responses, and that’s probably because they’re the most concerned about their health and welfare because they’re an at-risk population with COVID-19.”
How to get patients back
Hospitals also have to do more on their end if they want patients to come back, according to Wiik. There are three areas where they need to prepare for: PPE, testing, and staffing.
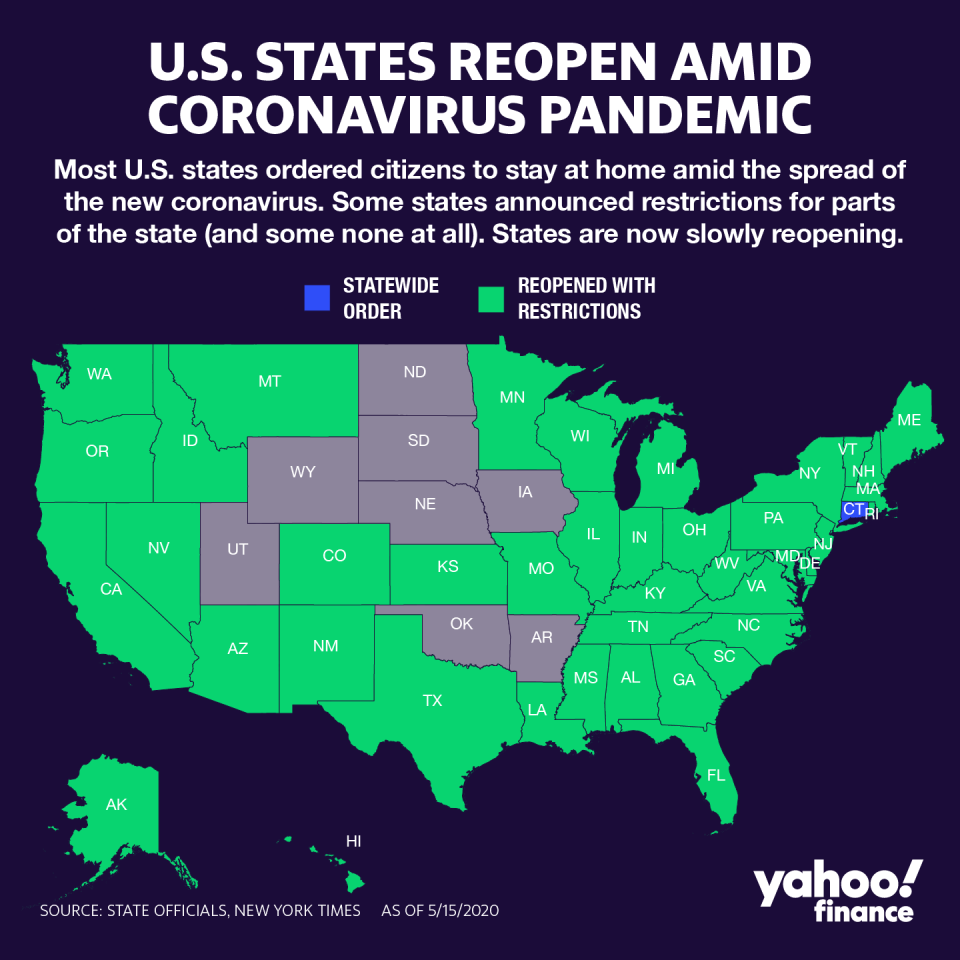
“I think hospitals are pretty prepared and providers were pretty prepared to get back as soon as they could at that point,” Wiik said. “If they were in a state like Nevada perhaps or Arizona, even Colorado for that matter, they may or may not have had surgery patients, but they’re coming back. They’ve got to meet those requirements and those milestones that are outlined, but the 14-day transmission rate has to go down, the PPE supplies have to be there, and that’s because the burn rate of PPE is much, much higher in an OR than it would be in a COVID ward. You’re going through quicker, procedure after procedure after procedure.”
In terms of testing, Wiik described it as a “headwind” that’s more of a federal and national issue.
“Then, finally, what does your staffing look like?” Wiik said. “If you were a furloughed hospital for example… you’ve got to get that staff back depending on what that arrangement is.”
Even if hospitals are able to meet these requirements, things aren’t going to go back to normal for several months.
“It’ll be closer to mid-June and late July before we start seeing 50 to 75% volumes return,” Wiik said, “simply because they’ve got the challenges of getting all those internal operations going, and then secondarily… you’ve got patients that want to come back and ones that are a little concerned about coming back. They’ve got to proactively reach out to them and get them engaged.”
Adriana is a reporter and editor for Yahoo Finance. Follow her on Twitter @adrianambells.
READ MORE:
Coronavirus pandemic 'threatens to make the opioid crisis substantially worse'
Coronavirus response: 'Someone has to pay' for the rising U.S. health care costs
Read the latest financial and business news from Yahoo Finance
Follow Yahoo Finance on Twitter, Facebook, Instagram, Flipboard, SmartNews, LinkedIn, YouTube, and reddit.

 Yahoo Finance
Yahoo Finance 

